All Issues
One in three suffers foodborne illness annually. Safeguarding food quality: a national priority
Publication Information
California Agriculture 48(1):7-12.
Published January 01, 1994
PDF | Citation | Permissions
Abstract
Foodborne illness is a relatively common occurrence. It is estimated that one third of the U.S. population suffers from foodborne illness each year and, according to the Centers for Disease Control and Prevention, about 9,100 die. These illnesses have been attributed to contaminating microbes, plant toxins such as pyrrolizidine alkaloids in herbal tea and plants, pesticide and antibiotic residues and microbes that have become antibiotic-resistant.
Full text
Microbial contamination resulting in serious foodborne illnesses has been associated with melons, tomatoes, asparagus, apples, potatoes, mushrooms, lettuce, eggs, meat, dairy products and seafood, among other foods.
Beginning in December 1992, the outbreak of E. coli 0157:H7 in 500 people in the northwestern United States focused the public's attention on the magnitude and lethal potential of microbially contaminated foods. Since January 1993, there have been no fewer than six outbreaks of E. coli 0157:H7 foodborne illnesses in the western United States. Similar foodborne outbreaks have been associated with a variety of other microbes such as salmonella, campylobacters, yersinia, among a multitude of other microbes. In this article, the food chain, food inspection system, examples of foodborne illnesses and potential ways to prevent foodborne illnesses will be addressed.
The food chain
The food chain has become more complex as our society becomes more urbanized and the food system more specialized. Factors that have increased the potential for food contamination include larger production units, specialized production practices such as calf raising, heifer raising and the use of chemicals to control infections in confined farming operations, and the consumer's interest in international cuisine. Figure 1 illustrates the modern day food chain. The pre-harvest portion of the food chain consists of the animals on the farm and their transport to the processing plants. The postharvest food system consists of the processing plant, wholesale distributors, retail preparers such as grocery stores or restaurants, and finally the consumer's home.
Contamination can occur at any point within the system (fig. 1). Most contamination, be it microbial or chemical, occurs initially on the farm (fig. 2). Microbes such as salmonella picked up on the farm are often the source of infection for other animals in the feed yard, during transport and at the processing plant. Cross contamination of carcasses may occur in processing plants if carcasses, equipment and utensils are not handled properly. Further contamination may occur as meats are prepared at wholesale distributors. A single piece of contaminated meat in a restaurant can serve as a major source of contamination if the meat is not well cooked and if the utensils used to prepare the meat are not cleaned and disinfected before use on other foods. This cross contamination is capable of causing large numbers of people to become exposed to potential disease-causing organisms.
The complexity of the food chain is illustrated by the fact that there are 913,000 cow-calf farms in the United States. Calves from these 913,000 farms are often transported to one of the 46,851 feed lots for fattening. The cattle from these feed lots then go to one of 81 processing plants that handle 90% of the cattle that end up as meat for U.S. consumers. If the meat ends up as hamburger, it could be served in some of the 146,000 fast food restaurants in the United States.
E. coli 0157:H7
E. coli 0157:H7 is the abbreviation of Escherichia coli 0157:H7. This microorganism is one of over 2,000 different strains of E. coli that may be found in humans, many of which play important roles in helping degrade and digest the foods we eat. E. coli 0157:H7 was first recognized as a cause of hemorrhagic uremic syndrome (HUS) in 1982, following a major outbreak of disease associated with eating undercooked hamburgers from a McDonald's fast food restaurant chain. Since that time, the disease appears to have increased in human populations in the United States, Canada, Europe, Argentina and elsewhere. E. coli 0157:H7 is now considered the second or third most important cause of foodborne illness in the United States. Since the microorganism was rarely observed prior to 1987, scientists think that it evolved from a progenitor strain in the 1970s. It is a new and emerging disease threat.
The disease
E. coli 0157:H7 is known to cause natural disease only in humans. There is no evidence that it causes disease in animals. The young, usually under 7 years of age; the aged, over 65 years of age; and those who are immunocompromised from cancer or chemotherapy are most likely to develop severe forms of disease. The onset of disease occurs 3 to 8 days after consuming contaminated food. The disease starts with abdominal cramping and diarrhea. On the second to third day of illness, bloody diarrhea appears and, in some cases, vomiting. Many individuals will recover; however, a few (8 to 10%) develop HUS or thrombotic thrombocytopenic purpura (TTP). TTP is a condition that depletes the platelets, resulting in widespread bleeding because the blood does not clot. These conditions are life threatening because they can lead to kidney failure, widespread bleeding and shock.
The E. coli 0157:H7 strain causes its destruction by attaching its long hairlike structures, called fimbriae, to the cells lining the intestine. Most of the E. coli 0157:H7 strains that cause disease produce toxins known as verotoxin I and verotoxin II. These toxins are capable of killing cells and causing diarrhea; bloody streaks or massive blood may appear in the stool. The genes that carry verotoxin I and II were introduced to the E. coli bacteria by virus-like particles known as phages. Phages are a common component of the microbial system just as viruses are common in mammals. At present there is no feasible way of controlling phages. Once the E. coli 0157:H7 bacteria has these toxin genes, they can be passed on to future bacterial generations. In addition, the phages can transfer the toxin genes to other bacteria.
E. coli: 500 cases of illness
The recent outbreak of E. coli 0157:H7 infections affecting over 500 people and causing four deaths in the northwestern United States was associated with the ingestion of contaminated hamburger from Jack In The Box restaurants. The exact source of the contaminated meat was never determined because of the complex procedures used to provide the restaurants with the formulated hamburger that the chain had requested. Formulation of products such as hamburger is important for taste, consistency and fat content. Jack In The Box had contracted with a wholesale/retail distributor for their hamburger. The wholesale/retail distributor subcontracted a firm to prepare the patties to meet the specifications for lean/fat content that Jack In The Box requested for the children's hamburgers. The multiple sources of the meat for the hamburger included beef from Australia, Colorado, California and possibly other states. The meat was then mixed together in large meat grinder mixers from which the patties were made. Some of these mixers may handle 4,000 to 6,000 pounds of meat at a time.
The grinding and mixing of meat with different lean/fat ratios for hamburger tends to fold and distribute the E. coli 0157:H7 throughout the patty. Hamburger must be cooked thoroughly throughout the patty to kill the microorganisms. The distribution of bacteria is different in steaks and whole pieces of meat, where the contamination tends to remain on the surface of the meat. Cooking temperatures of 166°F (74.4°C) are now required to kill E. coli in hamburger. At the time of the outbreak, hamburgers at Jack In The Box were cooked at 145°F (62.7°C), which was insufficient to kill the bacteria. Whole pieces of meat that have been contaminated, if cooked properly on the surface, have much less risk of causing disease because the heat kills the microorganisms during the cooking process. Appropriate cooking of hamburger means that there is no pink in the center of the patty and the juices are no longer pink.
Cattle carrying microbes can be a source of infection for other animals in feedlots (above) as well as during transport and at the processing plant.
Residues, antibiotic resistance
The public has expressed concern about the presence of manufactured chemicals such as antibiotics and pesticides in foods of animal origin. Much of this concern is based upon results of tests that have demonstrated that some chemicals are capable of causing cancer in laboratory animals.
In actual fact, the amount of manufactured chemicals that enter the food chain represents one tenth of 1 percent of the total toxic chemicals that we consume each day. The remaining 99.9% are naturally occurring toxins from plants and other sources (table 1). These natural toxins are the plants' means of protecting themselves from pests such as insects or microbial organisms. ( See p. 20 ). Fortunately animals that consume many of these plants are very efficient in neutralizing or destroying the toxins in their forestomachs or in their livers. The meat or animal products that consumers eat have less natural toxins than plant products such as vegetables and fruits because of the animals' natural detoxification systems.
The chemical residues that have received the most attention in animal products to date are antibiotics. Antibiotics have been used on animals to treat serious illnesses, as growth promotants and as feed additives to control infections. Most livestock and poultry receive probiotics or antibiotics at some time during their lives. The vast majority of animals are taken off treatment for extended periods before they or their products go to processing plants.
The use of antibiotics to treat life-threatening illnesses has been important for saving the lives of many animals. Antibiotics used for growth promotion and for controlling low-grade diseases are often included in feeds.
The medical community has been concerned about the use of antibiotics because it believes that antibiotic-resistant bacteria result from antibiotic overuse. Antibiotic resistance comes about because resistant genes are transferred from one bacteria to another through plasmids. Plasmids are viruslike particles that transfer genetic material from one bacteria to another. Humans are thought to acquire the resistant bacteria from eating animal products. However, proper cooking will destroy plasmids. The problems arise if a human patient acquires a life-threatening infection and the physician prescribes an antibiotic that is ineffective because the patient's bacteria have acquired antibiotic-resistant plasmids. The consequence may be death of the patient because the infection cannot be controlled. There is no definitive, only speculative, evidence that this has occurred. Scientists have noted an increasing incidence of antibiotic-resistant microorganisms in animals that has led to the speculation that the failure of humans to recover may be associated with the wide use of antibiotics in animals. There have been some suggestions that the E. coli 0157:H7 may have resulted from excessive use of antibiotics; however, there is no evidence that this has occurred.
Another concern of the medical community is that the presence of antibiotic residues in foods may lead to sensitization and eventual allergic reactions after a physician administers an antibiotic. Again, this concern is only speculative, and there is no direct evidence that this means of sensitization occurs.
Antibiotic residues are often detected in animals that have been recently treated for infections. Presently, most antibiotics can be purchased over the counter in drugstores or animal feed stores. Anyone can purchase these drugs. Although the instructions for administering the antibiotic are written on the label of the package, farmers often use antibiotics as they see fit – sometimes overtreating the animal, according to veterinarians and Pasteurized Milk Ordinance officials who investigate violations. In addition, livestock and poultry farmers often want to send animals to processing plants as soon as possible after they decide that the animals are not going to recover or when the cost of treatment is beyond the margin of profit that can be realized from the sale of the animal. Often these animals have significant quantities of antibiotics in their system. Antibiotics will eventually be eliminated from the body; however, the amount of time required to clear the animal's liver and kidneys depends on the individual antibiotic. The instruction labels on all antibiotics approved for use in food animals specify the amount of time that it takes for the drug to pass out of the animal. However, if animals or milk containing chemical residues reach the processing plants, the antibiotic is on its way to entering the food chain. The only way that antibiotics can be prevented from proceeding through the food chain is to stop the product from going forward.
The Food and Drug Administration (FDA), the Food Safety Inspection Service (FSIS), various national and state commodity organizations and individual farmers have undertaken efforts to recognize and eliminate antibiotic residues from the food chain. The federal agencies have initiated testing programs that will detect antibiotics in the slaughterhouses and milk processing plants. These tests are performed on random samples. This testing has greatly reduced the number of antibiotic-contaminated products that show up at the plants. FSIS, which monitors processing plants for 17 different antibiotics, currently reports a 0.42% violative residue rate. Contaminated carcasses are removed from the food chain.
The consequences for the farmer supplying contaminated products are significant economic losses. For instance, if animals are condemned, the farmer loses the sale, while in the case of milk, the whole tanker truckload is condemned and the owner(s) forfeits payment for the entire load. A milk tanker truckload represents a $5,000 to $6,000 economic loss. In addition, the dairy industry and federal government can revoke the license to sell milk for 2 days on the first offense, 4 days on the second offense, and if three violations occur, the license to sell milk can be revoked for as long as 1 year. The dairy industry has initiated a quality assurance program that includes the above stated penalties. These efforts by commodity organizations and individual farmers have greatly reduced the occurrence of chemical residues in animals and animal products. The other commodities have not effected programs with penalties for those producers that continue to send animals or products with violative levels of antibiotics to the processing plants.
USDA promotes safe handling of meat
On December 28, 1992, a 6-year-old San Diego girl, infected with the bacterium Escherichia coli 0157:H7, died within two weeks of eating a fast food hamburger. By the end of February 1993, over 500 laboratory-confirmed cases of the foodborne illness, resulting in three more deaths of children in Washington, Nevada and Idaho, were reported. The outbreaks were linked to E. coli present in ground beef served by Jack In The Box restaurants. The meat was traced back as far as the slaughterhouses – five in the United States and one in Canada were identified as the likely sources of the contaminated beef.
In March, several patrons of Sizzler restaurants in Corvallis, Grants Pass and North Bend in Oregon were sickened by E. coli 0157:H7, which was traced back to sauces and salad dressing containing contaminated mayonnaise. In August, a Sizzler in Seattle, Washington, closed after six patrons – five women and a 5-year-old boy – fell ill from food tainted with E. coli. In October, Texas officials reported the deaths of two children due to a complication associated with E. coli whose source has not been identified.
In February 1993, Secretary of Agriculture Mike Espy reacted by asking the Food Safety and Inspection Service to accelerate its plans to modernize its meat and poultry inspection, switching from relying on inspectors' visual observations to a science and risk-based system. He said that the 1907 inspection law is outdated and cannot adequately protect public health from microbial contamination today.
Inadequately cooked hamburger contaminated with E. coli 0157:H7 contributed to the illness of more than 500 people and the deaths of four children.
Espy also endorsed a program to reduce pathogens. One approach is helping producers prevent their livestock from becoming carriers of dangerous bacteria (see critical control point approach discussed on p. 12 ). The FSIS has stepped up its efforts to educate food handlers and consumers and has proposed a rule mandating that all raw meat and poultry products be accompanied with safehandling and cooking instructions.
Effective October 15, 1993, the USDA required the food industry to put safe-handling labels on ground or chopped meat. The industry has until April 15, 1994, to comply with new labeling requirements for all other uncooked meat and poultry products. In the meantime, all raw products must be accompanied by information, in the form of labels or leaflets, about safe handling of raw meats and poultry.
The enforcement of this rule was later called into question when a federal judge ruled that the USDA departed from normal procedures in mandating the labels. The department plans to write new rules for safety labels on meat, rather than pursue the matter in court.
—Editor
Quality assurance programs
Until recently, there were no control or monitoring programs for any chemicals or microorganisms. A systematic approach for identifying the source of entry of a contaminant into the animal and a means of monitoring for these potential contaminants was needed.
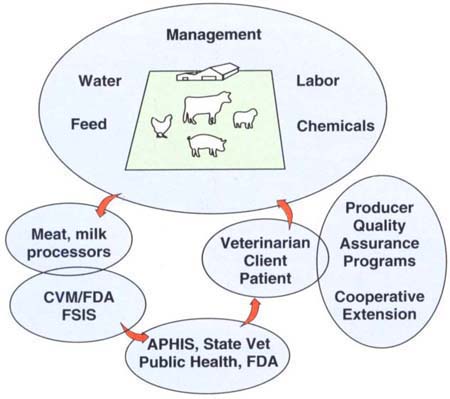
Figure 3 represents a schematic model that depicts the various constituencies that need to be involved in a producer-initiated quality assurance program. This type of program has been initiated in California by the UC Davis School of Veterinary Medicine, UC Cooperative Extension, the dairy industry, FDA, the USDA Animal and Plant Health Inspection Service (APHIS) and the California Department of Food and Agriculture's Bureau of Veterinary Services. It requires the farmer to follow a set of control principles and to keep accurate records.
Nationwide monitoring and inspection is performed by a small number of inspectors working for the Food Safety Inspection Service (FSIS) FDA's Center for Veterinary Medicine (CVM) and FDA's Center For Food Safety & Applied Nutrition (CFSAN), which monitors milk. This occurs only after the products arrive at the processing plants, as FSIS's and CVM's inspection responsibilities are limited to the processing plants. In most states, the state veterinarian, local FDA officials and public health officers are also notified of the violations. In some states, the state commodity quality assurance (QA) program officials are also notified as they are in a position to withhold or revoke the QA certification of the producer. In the proposed model, the veterinarian becomes a key person along with the producer in carrying out an investigation to determine where the system has failed.
The veterinarian is well positioned to help farmers reduce or eliminate contaminants from animals before they enter the food chain.
By using the systematic critical control point approach to evaluate the system and review data, it will be possible to determine where the system has failed. Both the producer and veterinarian must work closely with quality assurance program coordinators and extension personnel to ensure that the program objectives are met.
The veterinarian and producer must work closely in this program. The veterinarian, because of his or her training in health, is in an excellent position to provide leadership in managing preventive procedures to reduce or eliminate contaminants from the system. The veterinarian will certify products leaving the farm gate and can serve as a credible third party, ensuring that animals and their products have been handled in a prescribed manner.
A mandatory certification program that can be used by participating veterinarians is recommended as a critical element of the overall quality assurance program. Such a program would have significant value nationwide because it would put the farmer in charge of quality control at the front end of the process.
There are important roles for federal agencies to play in the interactions between the regulators and the producers or veterinarians. Presently, dairy farmers are notified by letter from the CVM that they are in violation. It is then up to the producer to make arrangements to correct the situation. APHIS and possibly state veterinarians could facilitate the process by serving as the principal vehicle for providing the information to the producers or veterinarians. APHIS personnel are well trained in these duties. In addition, they are in a position to assist in collecting and analyzing data, providing guidance on risk assessment and facilitating the program objectives. It is important that public health officials be informed just in case a human health crisis occurs.
A producer wishing to initiate a quality assurance program often needs guidance. This can be provided by facilitators whose primary objective is to introduce the producer to the program through an educational process. A facilitator can be a local veterinarian, an APHIS veterinarian, Cooperative Extension personnel, or individuals from the Quality Assurance Board. This type of voluntary program is an alternative to an enforceable regulatory program. The basis for this type of program is economically driven. The product leaving the farm gate, if meeting certification standards, should qualify as a value added product. Processors and consumers can be assured that the risk of microbial or chemical contaminants is low or nonexistent.